The Star*D Trial was a nationwide study to find out the overall efficacy of antidepressants and psychotherapy for treatment of major depressive disorder. The study reported that one third of depression patients did not respond to the use of multiple antidepressants across different classes. Also, after the failure of the first antidepressant, the subsequent antidepressants showed much less response to the use of subsequent antidepressants.
Side effects of antidepressant medications:
Pharmacogenetic evidence suggests that a significant number of individuals have a high intolerance to antidepressants. They may be predisposed to severe side effects from antidepressants because of specific genetic predispositions resulting in very slow removal of the drug from the body or specific changes at the receptor levels. They are likely to give up the use of medications after suffering from severe side effects.
Can antidepressants stop working?
It is frequently observed that antidepressants may work consistently for a while and then lose their effectiveness altogether. Depression results from complex interactions of genetics, life experiences, ongoing life stressors, medical illness and the changing brain and body mechanisms with age. The medications which worked for some time may seem no longer effective under different set of conditions.
Treatment resistant depression (TRD):
To stop or continue the use of antidepressant for TRD?
For some people with treatment-resistant depression, antidepressants may generally have little or no positive effect on one’s depression symptoms, which, combined with possible long-term undesirable side effects, may further worsen one’s mood and quality of life. Any changes in medications for TRD should be done carefully under the guidance of a psychiatrist.
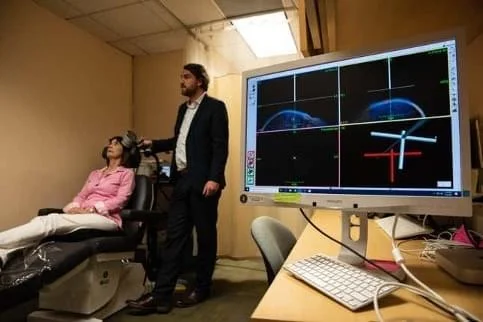
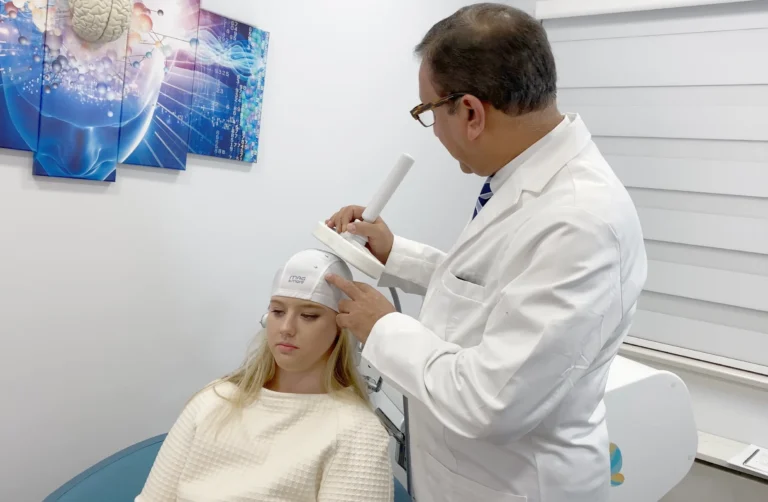
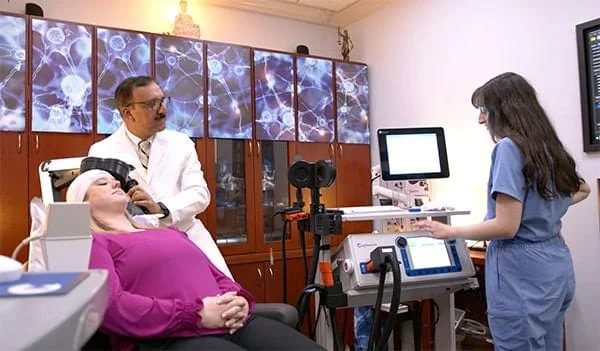
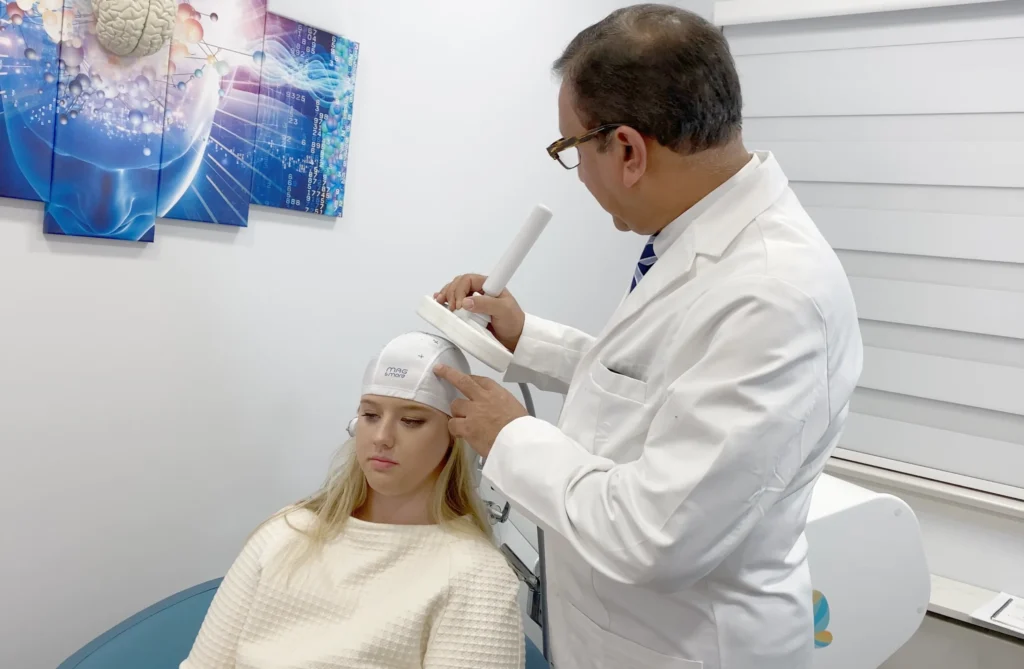
TMS Therapy for treatment-resistant depression
TMS therapy for depression uses magnetic pulses to the left prefrontal cortex of your brain—the part responsible for mood regulation. Magnetic pulses produce very small electrical currents in the brain regions resulting in a number of local effects like: stimulating brain cells to release neurotransmitters, increasing blood flow, enhanced neuronal connectivity and neuroplasticity.
Just like an MRI scan, TMS therapy is generally a painless procedure. There are very few side effects, mainly scalp discomfort or mild headache in the first week. There are no reported harmful side effects to the brain and there are no systemic side effects, as caused by medications. TMS patients can get right back to their daily routine with no impairment after a session.
While there is no cure for depression, TMS therapy is an extremely effective treatment for major depression when counseling and medication have both failed to yield positive results. The treatment response to TMS with recently improved protocols is over 70% in the majority of patients with depression.
If you have been diagnosed with major depression or an anxiety disorder, have exhausted all other possible treatments (considered treatment resistant depression), then TMS may be the next best treatment option for you, if you meet the criteria for TMS therapy. Sleep TMS & Wellness Center in Great Neck offers state-of-the-art TMS therapy on Long Island. It is supervised by Dr. Gupta, a neuropsychiatrist who is quadruple board-certified with over 25 years of clinical experience. STW center has two TMS systems, with above average outcomes from use of neuro-navigation and an excellent TMS staff.